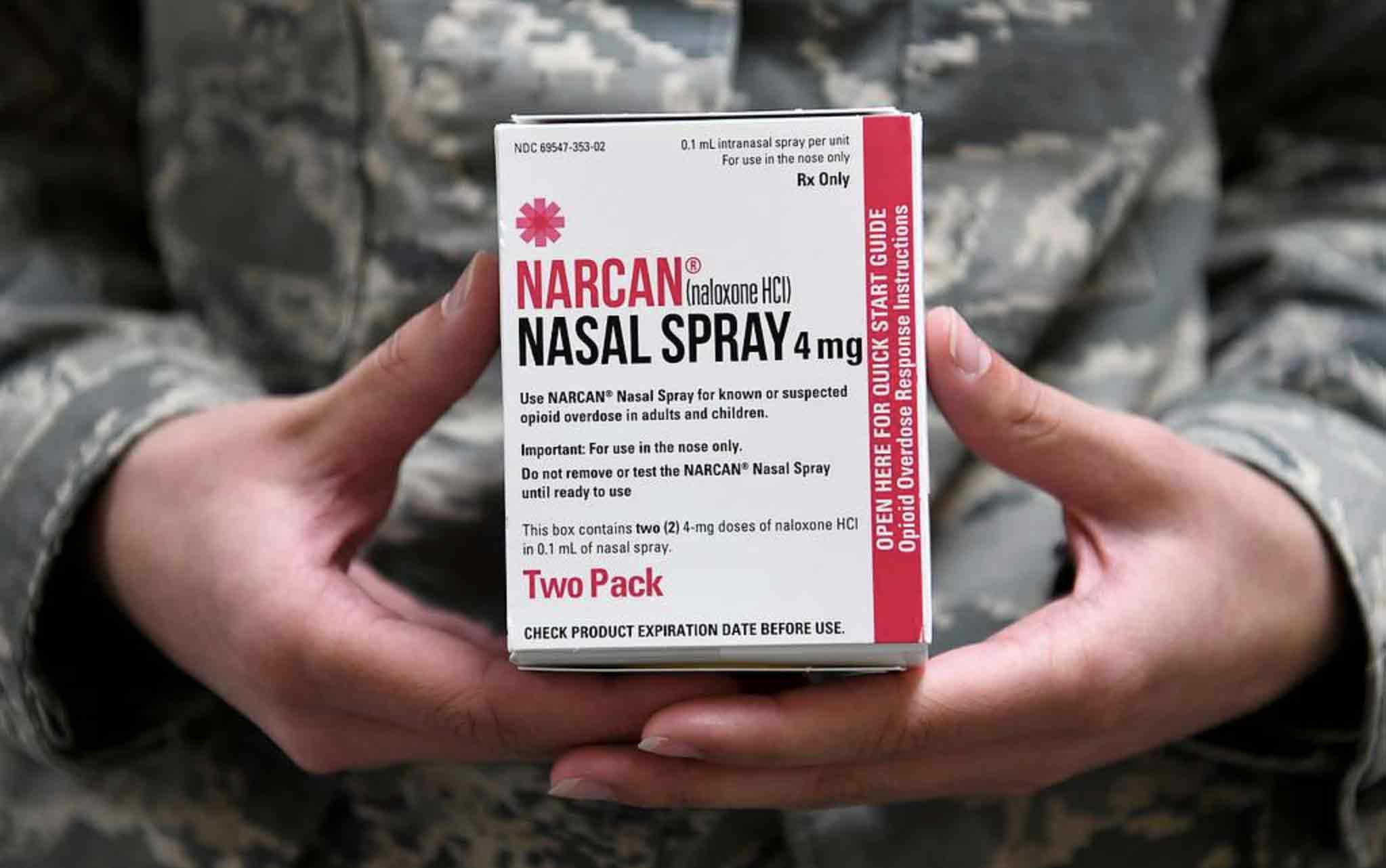
What is Nalaxone?
Naloxone (also known as Narcan®) is an FDA-approved medication designed for the swift reversal of opioid overdoses. Classified as an opioid antagonist, it functions by binding to opioid receptors, effectively counteracting and obstructing the effects of other opioids, such as heroin, morphine, and oxycodone. When administered to individuals displaying signs of opioid overdose, naloxone provides temporary relief, but its effects are short-lived. Therefore, it is of utmost importance to seek immediate medical attention following the administration or reception of naloxone.
This medication can be administered via intranasal spray (through the nose), intramuscular injection (into a muscle), subcutaneous injection (under the skin), or intravenous injection.
Healthcare practitioners should evaluate the necessity of prescribing naloxone for patients on methadone or buprenorphine treatment, as well as those at risk of opioid overdose.
Does Nalaxone Save Lives?
The impact of Naloxone on saving lives is difficult to quantify precisely, but there is substantial evidence to suggest that it has made a substantial difference. Emergency medical services and law enforcement agencies across the world have administered Naloxone in critical situations, often reversing overdoses before they become fatal. Furthermore, community-based programs, needle exchange sites, and harm reduction organizations have distributed Naloxone kits to individuals who use opioids and their loved ones. This widespread availability has empowered many to intervene during overdose emergencies, potentially preventing thousands of deaths annually.
However, while Naloxone is an essential tool in reducing opioid-related fatalities, it is not a standalone solution to the complex issue of opioid addiction and overdose. It must be part of a comprehensive approach that includes harm reduction strategies, increased access to addiction treatment, and addressing the root causes of opioid addiction. Nevertheless, there is no doubt that Naloxone has saved numerous lives, providing a vital second chance to individuals struggling with opioid use disorder, and offering hope for recovery and healing.
Understanding Opioid Overdose and Nalaxone
Naloxone’s primary purpose is to counteract the effects of opioid overdose, such as those resulting from morphine or heroin.
More specifically, naloxone is employed during opioid overdoses to reverse the life-threatening depression of the central nervous and respiratory systems, thereby restoring normal breathing in overdose victims. This prescription medication is categorized as nonscheduled, meaning it is non-addictive. Naloxone’s efficacy is contingent upon the presence of opioids in a person’s system; it remains ineffective when opioids are absent.
While traditionally administered by emergency responders, naloxone can also be administered by individuals with minimal training, making it an invaluable tool for addressing overdoses in individuals prescribed opioid pain medication and those using substances like heroin and other opioids.
Importantly, naloxone carries no potential for abuse. It can be injected into a muscle, vein, or under the skin, or sprayed into the nasal passages. Notably, injectable naloxone is available in a lower concentration (0.4mg/1mL) compared to the nasal spray version (2mg/2mL). Naloxone’s effects are temporary, wearing off within 20-90 minutes.
Eligible candidates for naloxone include individuals who:
- Depend on high doses of opioids for prolonged management of chronic pain.
- Have been discharged from emergency medical care due to opioid poisoning or intoxication.
- Utilize rotating opioid medication regimens.
- Take specific extended-release or long-acting opioid medications.
- Have undergone a period of abstinence from opioids, including those recently released from jail.
In the case of pregnant women, naloxone can be safely administered in controlled doses under the supervision of a healthcare professional.
Doctors or pharmacists can provide guidance to patients, their family members, or caregivers on how to administer naloxone effectively.
Patients using an automatic injection device or nasal spray should ensure it remains readily accessible at all times. It’s crucial to keep in mind to replace the medication once it reaches its expiration date or if it has been exposed to temperatures below 39°F or above 104°F.
Whaere to Find Nalaxone
The U.S. Food and Drug Administration (FDA) made a significant announcement on March 29, 2023, by granting approval for Narcan 4 milligram (mg) naloxone hydrochloride nasal spray as the first nonprescription naloxone product. After the finalization of this transition to over-the-counter status, this vital medication, crucial for reversing opioid overdoses, will be easily accessible to consumers in locations such as drug stores, convenience stores, grocery stores, gas stations, and through online channels.
Side Effects of Naloxone
It’s crucial to treat serious side effects seriously, as some may signal a medical emergency. Patients should cease taking naloxone and promptly contact a healthcare professional or emergency services.
Patients and healthcare providers are encouraged to report all side effects through the FDA’s MEDWatch program, an online platform for reporting medical product safety concerns, accessible to healthcare professionals, patients, and consumers. Alternatively, they can report by calling 1-800-FDA-1088.
Individuals who exhibit signs of an allergic reaction to naloxone, such as hives or swelling in the face, lips, or throat, should seek immediate medical attention. It’s important for them to refrain from driving or engaging in other potentially hazardous activities.
The use of naloxone can induce symptoms of opioid withdrawal. Seeking medical assistance promptly after administering or receiving naloxone is essential.
Opioid withdrawal symptoms encompass:
- Restlessness, nervousness, or irritability
- Unexplained sneezing or a runny nose in the absence of a cold
- Muscle aches
- Weakness or dizziness, vertigo
- Gastrointestinal discomfort, including diarrhea, stomach pain, or nausea
- Flu-like symptoms like fever, chills, or goosebumps
Opioid Overdose
Opioid overdose poses a grave, life-threatening situation that demands immediate emergency intervention. The ability to identify the indicators of opioid overdose is pivotal in preserving lives. Gain further insights into opioid overdose.
Opioid overdose may occur in the following circumstances:
- When a patient misinterprets medication instructions, inadvertently consumes an excess dose, or intentionally misuses a prescribed opioid.
- As a result of illicit drug consumption.
- When an individual ingests opioid medications meant for someone else.
- Through the combination of opioids with other medications, alcohol, or over-the-counter drugs.
Indicators of Opioid Overdose:
- The individual remains unresponsive to touch or voice, unable to wake.
- Abnormal breathing patterns, characterized by very slow respiration or cessation of breathing.
- Constricted, pinpoint-sized pupils.
- Bluish discoloration of the lips and nose
Most of us who deal with addiction need help to get sober, so don’t be ashamed to reach out. Call Ventura Recovery Center for a Confidential Consultation. (800) 247-6111.